Results from a new cross-sectional study published in Respiratory Medicine provide evidence that obesity is associated with adverse respiratory symptoms in women, but the same correlation was not observed in men.
Because obesity is a known risk factor for higher rates of new and worsening respiratory diseases such as asthma and chronic obstructive pulmonary disorder (COPD), Swedish researchers set out to investigate the association between abdominal and general obesity with respiratory symptom severity in asthma and COPD in adult men and women.
Design
The Swedish study relied on patient data from the Respiratory Health in Northern Europe (RHINE) III questionnaire, which contained the health records of 12,290 individuals over two years, from 2010 to 2012. The self-reported questionnaire included questions such as ‘Have you had an asthma attack in the last 12 months?’ and ‘Do you usually cough up mucus in the chest that is hard to get out?’ The study also used self-reported body mass index (BMI), where general obesity was defined as BMI ≥30kg/m2 and abdominal obesity was defined as a waist circumference (WC) of ≥ 102cm in men and ≥88cm in women.
Results
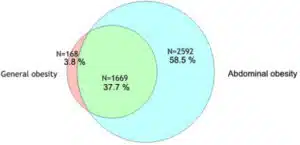
Of the participant data used, it was found that 34.7% had abdominal obesity, 6.7% had general obesity, and 13.6% had both abdominal and general obesity (see graph). Both abdominal and general obesity were independently associated with respiratory symptoms with an odds ratio (OR) of 1.25 to 2.00 in both adult women and men. Asthma was significantly associated with abdominal obesity (OR, 1.56; 95% CI, 1.30-1.87; P = .052) and general obesity (OR, 1.95; 95% CI, 1.56-2.43; P = .006), respectively, in women, but not in men. Similarly, COPD was significantly associated with abdominal obesity (OR, 1.62; 95% CI, 1.15-2.28; P = .02) and general obesity (OR, 2.87; 95% CI, 2.00-4.10; P = .001), respectively, in women, but not in men.
Limitations
The study was based on a self-reported questionnaire, but the researchers believe that their results provide a clearer picture when treating female patients with respiratory symptoms and obesity. It is also notable that abdominal obesity was more common in the women who participated, while the men who responded had higher rates of general obesity than women. This gender-specific observance, specifically the link between abdominal adipose tissue and breathing issues in women, may be worthy of further exploration. Lastly, the researchers identified three lifestyle factors (smoking, education, and physical activity level) as possible confounding variables in their study.
Discussion and Takeaway
The clinical relevance of the correlation uncovered by Dr. Kisiel and his colleagues may result in providers measuring WC in addition to height and weight when seeing patients with respiratory symptoms. The researchers concluded their publication by stating that both general and abdominal obesity independent of each other were associated with respiratory symptoms, but “for self-reported asthma and COPD, a significant association with abdominal and general obesity was found in women but not men. Measuring waist circumference can be important when seeing patients with respiratory symptoms. General and abdominal obesity were independent factors associated with respiratory symptoms. Asthma and COPD disease were independently linked to abdominal and general obesity in women but not men.”
“The main result of this study was that both general and abdominal obesity were independently associated with respiratory symptoms in adults. However, asthma and COPD were significantly associated with abdominal and general obesity in women only.” – Kisiel, et al.
Source
- Kisiel MA, Arnfelt O, Lindberg E, et al. Association between abdominal and general obesity and respiratory symptoms, asthma and COPD, results from the Rhine study. Respiratory Medicine. 2023;211:107213. doi:10.1016/j.rmed.2023.107213