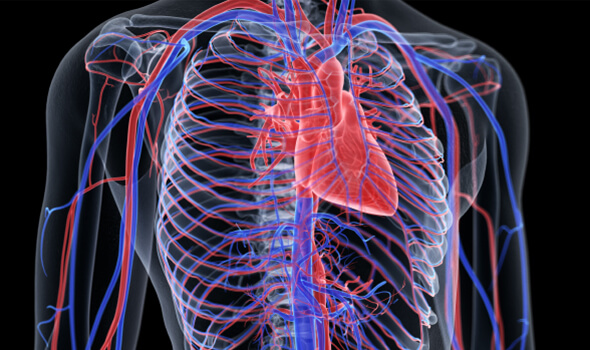
RAAS inhibitors either reduce angiotensin II synthesis, thereby inhibiting aldosterone secretion (ACEIs), or may impair the angiotensin II receptors (AT I) (ARBs). The CCBs reduce blood pressure by relaxing vascular smooth muscle and dilates blood vessels, and therefore, reduce peripheral resistance. The diuretics, on the other hand, curbs sodium and water retention by the kidneys and hence, reduces extracellular fluid volume.
Hypertension lies at the crossroads of significant health complications- cardiac dysfunction, stroke, and renal disorder. The diuretics, a prominent class of medication prescribed to treat hypertensive patients, targets kidney function by tightly regulating sodium and water load; they affect the renal tubules of the kidney to expedite their release from the body. According to the ACC/AHA guidelines, the diuretics are incredibly favorable for patients with diabetes, >65 years of age, of African origin, with a history of stroke or low renin, and even people who have suffered from cardiac failure. The thiazide-type diuretics constitute the only category of diuretics that dilates blood vessels, in addition to regulating sodium and water retention in the body, thereby reducing blood pressure. Though the precise functional mechanism is unknown, these diuretics target the distal convoluted tubules in the kidney. Several meta-analyses and clinical studies (on patients with varied medical histories) have tested the efficacy of the thiazide-type diuretics. These diuretics have exhibited favorable outcomes in these studies; their effectiveness proved to be comparable with other classes of hypertension medications.