On Wednesday, Oct. 18, 2023, Cardiometabolic Health Congress (CMHC) returned to the Boston Park Plaza for the 18th Annual Conference, Social Determinants and Digital Advances in Cardiometabolic Health. The preconference day focused on the increasing interest in digital health tools to improve health outcomes in cardiometabolic diseases such as diabetes, obesity, hypertension and arrhythmia.

Opening Remarks
Seth S. Martin, MD, MHS, took the stage to welcome an international audience of multidisciplinary providers to the preconference kick-off for Social Determinants and Digital Advances in Cardiorenal Metabolic Health. He remarked that the decision to focus the entire first day on digital health was a “Culmination of the energy, excitement, and relevance of this topic to clinicians.” He welcomed the morning’s incredible lineup of expert faculty, noting their shared goal to improve and prolong life represents a bright spot amid the dark events happening around the world.
Setting the Stage: What Digital Health Means for Clinicians and Patients
When Patrick Dunn, PhD, MS, MBA, took the stage for his session on practical applications for digital health software in daily clinical practice, he opened by stating that the current field is in an exciting time where the vast amount of data and computing power have made technologies that were once a fantasy into a reality. In his role as program director of the Center for Health Technology and Innovation at the American Heart Association (AHA), Dr. Dunn noted that health technology collaboration is a two-way street. Scientists and clinicians must work to make sure the data used to train models is accurate and unbiased, and the tech side must be diligent in making sure the software and platforms are being used correctly in practice.

"For AI to be successful, it needs to be supportive but subordinate to human thinking. The data needs to be transparent, and we need to establish best practices and build evidence-based solutions for scalable, sustainable models that both clinicians and patients can trust."
Dr. Patrick Dunn
Health and Care Apps for Lifestyle and Obesity: The Importance of Self-Monitoring
To begin the sessions on using digital health and lifestyle interventions to manage obesity, Dr. Martin welcomed Tiffany Powell-Wiley, MD, MPH, to the podium. In her role overseeing social determinants of obesity and cardiovascular risk for the National Heart, Lung and Blood Institute, Dr. Powell-Wiley is an expert in how self-monitoring apps can help patients from at-risk populations manage their weight and adopt healthy lifestyle changes. She addressed how building datasets from diverse populations can equip artificial intelligence (AI) platforms and other digital health technologies better to represent patients from vulnerable or under-served communities.
"Self-monitoring health apps are great for most consumers, but they have limitations in terms of vulnerable populations not being represented in product development. Because data from racial minority or at-risk populations isn't used to create the model, it is unlikely the finished product will address the specific needs of those patients."
Dr. Tiffany Powell-Wiley

Continuous Glucose Monitoring: The New Frontier in Lifestyle Management?
To build on the day’s preconference theme of using health technology to improve outcomes in patients with cardiometabolic and cardiorenal conditions, Athena Phillis-Tsimikas, MD, delivered a presentation on using continuous glucose monitoring to implement behavior change. Dr. Phillis-Tsimikas presented evidence that, when exposed to their own real-time glucose readings, patients were motivated to implement lifestyle changes that resulted in moderate weight loss and better glucose control.
"We can detect prediabetes very early using continuous glucose monitoring because it picks up even slight glucose dysregulation. This allows us to personalize a diet for optimal glucose response before a patient even develops symptoms of prediabetes."
Dr. Athena Phillis-Tsimikas
Changing Behavior Using Digital Health for Long-Term Weight Management
When Dr. Martin introduced the next speaker, Martin S. Hagger, PhD, he pointed out that his scientific affiliation with multiple universities was a likely reflection of his collaborative spirit. As a behavioral scientist with a dedicated research lab at the University of California Merced, Dr. Hagger shared many insights on how digital health tools can result in significant and sustainable weight loss, delving into the psychological aspect of altering behavior.
"Many health outcomes for both communicable and noncommunicable diseases are rooted in behavior, whether it be people engaging in behaviors that pose a risk, or refraining from behaviors that aid in prevention."
Dr. Martin S. Hagger
Panel Discussion and Audience Q&A
To put the topics presented thus far into context, the experts returned to the stage for a lively and candid panel discussion on how to practically apply these digital technologies. Then, the faculty answered questions submitted by audience members via iPads and discussed the advantages and pitfalls of using various forms of technology to monitor and manage their patients.

The Role of CGM in the Management of Type 2 Diabetes: Patient Selection & Important Pearls
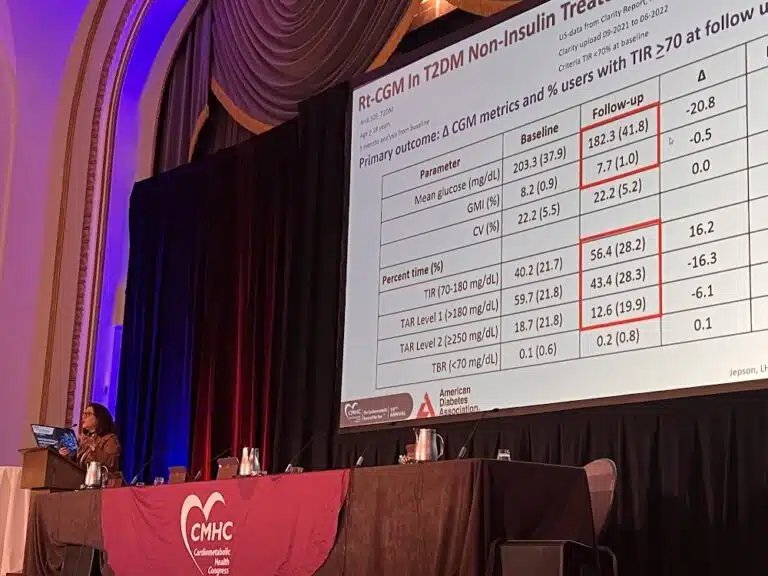
After a brief break in sessions, during which attendees mingled and enjoyed refreshments in the exhibit hall, Grazia Aleppo, MD, presented data on why it is so important for patients to be educated on the use of continuous glucose monitoring in order to use the technology successfully. She pointed especially to evidence that the younger a patient is when they are diagnosed with diabetes, the more likely they are to die at a younger age. Because the technology to manage diabetes is available, she urges clinicians not to wait until they see an A1c of 12% to initiate therapy. “Let’s get to that patient when the A1c is still 5% or 6%, and that may mean they are prescribed this technology by their primary care physician before they need a specialist.”
"We know that when continuous glucose monitoring begins in primary care the results are fantastic. Let's encourage our primary care colleagues to familiarize themselves with this technology and have confidence in prescribing it to their patients early."
Dr. Grazia Aleppo
Insulin Delivery and Insulin Pumps in Patients with Type 2 Diabetes
Building on Dr. Aleppo’s lecture on continuous glucose monitoring technology, Viral Shah, MD, led an insightful session on the use of novel insulin delivery systems. He opened by remarking that “The onus is on us as providers to understand the technology.” Comparing the new waves in diabetes technology to waiting for a new iPhone model each year, Dr. Shah stressed that, while armed with enough evidence to gain regulatory approval, more rigorous control trials are needed to better understand which patients are candidates for newer insulin delivery systems.

"It's not like these patients' only job is managing their diabetes. They have lives and responsibilities, so the challenge in managing both type 1 and type 2 diabetes is delivering a technology people can easily use to improve their agency and outcomes."
Dr. Viral Shah
Technology to Close Gaps in Hypertension Care
As the sessions pivoted toward how technology can improve cardiovascular outcomes, Daichi Shimbo, MD, was welcomed to the stage to discuss the public health crisis of rising hypertension in adults in the U.S. He noted that even after multiple U.S. guidelines were published and amid increasing public health interest in the dangers of unchecked hypertension, the numbers are moving in the wrong direction. A noninvasive cardiologist at the Columbia University Irving Medical Center, Dr. Shimbo argued that out-of-office (ambulatory) blood pressure is probably far more informative than a reading taken in the office. He advised the audience that the office visit is where you can get an estimate of what’s happening chronically with the patient but that remote monitoring technology, even for just a 24-hour period, is more highly predictive of adverse cardiovascular events and related mortality.
"The overall increase of 1 or 2 millimeters of mercury for systolic blood pressure seems quite small, but I just want to remind you from a public health point of view that even though those numbers are small for an individual person, I would argue for population they are quite huge, particularly for cardiovascular risk prevention."
Dr. Daichi Shimbo
Advances in Digital Health for Arrhythmia Management
“There is no one better than Mohamed Elshazly, MD, MBEE, to tackle the next topic of heart rhythm management,” said Dr. Martin as he welcomed his colleague to the stage. A cardiac electrophysiologist at the Medical University of South Carolina and director of Cardiac Electrophysiology at the Ralph Johnson VA Medical Center in Charleston, Dr. Elshazly began by presenting his definition of digital health as a “Modern device with hardware and software components that generate actionable health information.” He further distilled this definition of medical devices as falling into two buckets: consumer devices such as smartwatches, and clinical-grade devices that require regulatory oversight. With the former, he cautioned that although these devices are easy to access and use, they may have lower sensitivity and higher specificity than the clinical-grade devices. “This might seem decent,” commented Dr. Elshazly, “but if it results in even a 2% false positive rate of arrhythmia for everyone who wears an Apple Watch, that’s a lot of people getting false positives that can lead to unnecessary care and costs.”
Fireside Chat: Insights from Industry – Next Frontiers in Digital Interventions to Improve Cardiometabolic Health
The preconference ended with a sizzling session by the virtual fire, where a panel of experts representing organizations from academia, science, industry, business and drug development discussed using digital health solutions to address current gaps in cardiometabolic health.
Meet The Experts:

Seth S. Martin, MD, MHS
Director of the Center for Mobile Technologies to Achieve Equity in Cardiovascular Health at Johns Hopkins

Francoise A. Marvel, MD
CEO and Co-Founder of Corrie Health

Kapil Parakh, MD, MPH, PhD
Senior Medical Lead at Google

Grant Groves, PhD, MBA
Digital Health Asset Lead for Cardiometabolism at Boehringer Ingelheim

Stephen Lynch
Director of Digital Marketing at Novo Nordisk

Patrick Dunn, PhD, MS, MBA
Program Director of the Center for Health Technology and Innovation at the American Heart Association
These hard-hitters engaged in a collaborative panel discussion and fielded audience questions on how their organizations are tackling the current gaps in cardiometabolic health outcomes, and weighed in on future implications of digital tools for patients, clinicians, and the health care system at large.

Thank you to our attendees, faculty, staff and exhibitors for a wonderful first day of the 18th Annual CMHC at the iconic Boston Park Plaza! We’ll have more insights and highlights tomorrow, Thursday, Oct. 19, 2023, when the expert-led education continues.











